- Home
- Users & Science
- Scientific Documentation
- ESRF Highlights
- ESRF Highlights 2013
- X-ray imaging
- Development of new treatments for epilepsy using synchrotron radiation
Development of new treatments for epilepsy using synchrotron radiation
Epilepsy is the most common neurological disorder with an incidence reaching 0.5% of the population. About one third of the patients with epilepsy are affected by medically refractory seizures. These patients are exposed to the risk of severe traumatic, metabolic and neuropsychological sequelae and can die as a consequence of uncontrolled seizures. Epilepsy surgery aiming to resect the epileptic focus can provide seizure freedom to selected patients but there is a high risk of neurological complications when the focus involves the eloquent cortex, such as the language and motor areas, or the dominant hippocampus, a structure located in the mesial part of the temporal lobe exerting a crucial role in the genesis of new memories. For refractory epilepsy located in brain regions unattainable with conventional surgery, multiple subpial transections (MST) and stereotactic radiosurgery (SRS) are the most attractive [1] of the non-resective surgical approaches. MST is a microsurgical procedure placing vertical incisions through the epileptic cortex in order to cut the horizontal axons responsible for the propagation of seizures while preserving the vertical columns acting as the basic unit of cortical function. Seizure spread is arrested by the parcellisation and disconnection of the ictal focus. The cortical columns subserving eloquent and non-eloquent neurological functions are not injured by MST, allowing the treatment of epileptic foci located over sensorimotor or language cortex not amenable to surgical resection.
Focal irradiation of an epilepsy focus through SRS is an emerging treatment for medically refractory seizures, providing a non-invasive approach which is mainly limited by the delay of efficacy and side effects (several months are required to obtain seizure relief). However, current LINAC- or cobalt-based technologies do not allow high doses to to be delivered to cortical slices of millimetric size, thus replicating the exquisite cortical incisions generated by MST.
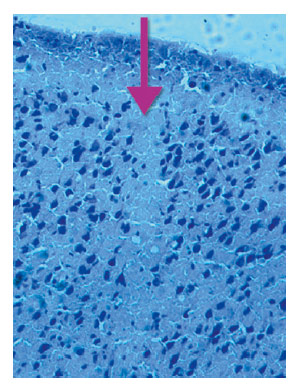
We have investigated a novel and exciting approach combining the advantages of SRS and MST at beamline ID17, where arrays of microplanar beams were used to generate cortical transections equivalent to MST in a non-invasive, bloodless way. These microscopic arrays of X-ray beams (microbeams) originating from a synchrotron source were used to generate neocortical or hippocampal transections by delivering very high doses of radiation to tissue slices of microscopic thickness. Neurons, glia and axons along the penetration path were ablated, leaving a path equivalent to that of a microsurgical incision (Figure 9). The adjacent tissue was exposed to much lower valley doses (less than 5 Gy) unable to induce histologically evident tissue damage [2]. In essence, synchrotron-generated cortical transections provide a microradiosurgical equivalent of MST. Compared to MST, which require an invasive procedure involving all the risks related to open surgery, microbeam transections are performed in a non-invasive way and the size and spacing of the transections can be modified by the surgeon according to the needs. We have also shown that microbeam transection of the primary motor cortex, a highly challenging target, is well tolerated. No sign of motor deficit was found after prolonged observation and periodic rotarod testing. Convulsive seizures originating from this region disappeared almost immediately after microbeam transections.
 |
|
Fig. 9: Synchrotron-generated sensorimotor cortex transection. |
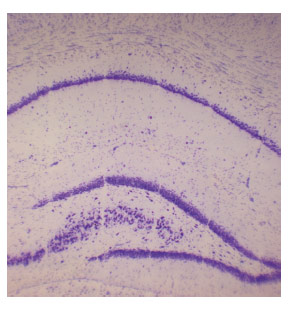
Seizure control and preservation of motor function after sensorimotor cortex transection are an exciting new application of synchrotron-generated microbeams, opening the way to the application of this new concept to the most common source of medically-refractory seizures, the hippocampus. We have investigated hippocampal transections in a rat model (Figure 10) and further studies are ongoing to characterise the ability of hippocampal transections to control seizures originating from this region.
 |
|
Fig. 10: Synchrotron-generated hippocampal transections. |
Microbeam transections hold a great potential to modulate cortical function and to treat focal epilepsy. Microbeam transections, either placed over neocortical seizure foci or through the hippocampus, could prove to be an excellent tool to be added to the current techniques used to control seizures. The development of devices delivering submillimetric beams able to generate cortical transections might add a powerful new tool to the clinical treatment of epilepsy and, more generally, to modulate cortical functions in a wide variety of neuropsychiatric disorders.
Principal publication and authors
P. Romanelli (a,b), E. Fardone (b), G. Battaglia (c), E. Bräuer-Krisch (b), Y. Prezado (b), H. Requardt (b), G. Le Duc (b), C. Nemoz (b), D.J. Anschel (d), J. Spiga (e) and A. Bravin (b), PLoS ONE 8, e53549 (2013).
(a) Brain Radiosurgery,Cyberknife Center,CDI, Milan (Italy)
(b) ESRF
(c) Istituto Di Ricovero e Cura a Carattere Scientifico Neuromed, Località Camerelle, Pozzilli (Italy)
(d) Comprehensive Epilepsy Center of Long Island, St. Charles Hospital, Port Jefferson, New York (USA)
(e) Department of Physics, University of Cagliari and Istituto Nazionale di Fisica Nucleare, Monserrato (Italy)
References
[1] P. Romanelli, P. Striano, M. Barbarisi, G. Coppola and D.J. Anschel, Epilepsy Res. 99, 193-201 (2012).
[2] P. Romanelli and A. Bravin, Neurol Res. 33, 825-31 (2011).



