- Home
- Users & Science
- Scientific Documentation
- ESRF Highlights
- ESRF Highlights 2011
- Structural biology
- The molecular mechanism of pain relief
The molecular mechanism of pain relief
General anaesthetics are one of the classes of medicine that have reduced human suffering more than any other drug. Despite widespread use, their exact mode of action is not well understood, but a growing body of evidence suggests that they bind specifically to membrane bound receptors in the synapses of nerve cells. These receptors, called pentameric ligand gated ion channels, send an electrical signal in response to a chemical signal. Two crystal structures of a bacterial homologue of these receptors, in complex with two general anaesthetics, have recently been solved (electrophysiological tests showed that this bacterial homologue is also sensitive to general anaesthetics). The results reveal a specific cavity in which the drugs are bound, offer insights into their molecular mechanism, and have the potential to allow the development of improved anaesthetics in the future.
Nerve impulses control processes in the body from movement to sight and thought. They are propagated between nerve cells by chemical signals transmitted across synapses. When an electrical potential arrives at a synapse in response to a stimulus, it must be transmitted across the synaptic cleft – the gap between nerve cells. This is an entirely chemical process, where the change in electrical potential triggers the release of neurotransmitters. These molecules then bind to pentameric ligand-gated ion channels (pLIGICs) in the membrane of the adjoining nerve cell. The binding of the molecules stimulates the opening of pLIGICs allowing the rapid influx of cations into the cell, which in turn propagates an electrical impulse along the nerve, thereby transmitting the stimulus. The channels produce local permeability changes in the membranes that are directly correlated to both the concentration of neurotransmitter and its lifetime in the synaptic cleft - changing a self amplifying electrical transmission into a highly-sensitive, graded response. Their receptors are the target of many psychoactive drugs and are probably also the targets of general anaesthetics, but, as they are membrane proteins, structural studies are challenging. Recently, a bacterial homologue of human pLIGICs was discovered and its structure solved [1,2], showing the first molecular details of this class of membrane protein and providing an excellent model for studies of neurotransmission.
 |
|
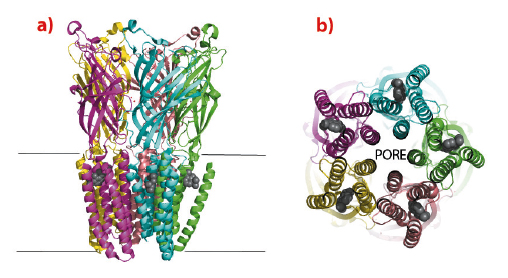
Fig. 101: The structure of a bacterial pLIGIC bound to the anaesthetic propofol. a) The channel is shown as a ribbon with each pentamer coloured differently, the position of the protein within the cell membrane is indicated by the two lines. Neurotransmitters bind in the extracellular domain and cause the opening or closing of the cation channel located in the membrane domain. Propofol is shown as Van der Waals spheres (grey) and is bound within the membrane domain of the protein. b) View of the channel from inside the cell. The cation pore is formed at the interface of the five subunits and is in the open conformation. Propofol (grey spheres) binds in a hydrophobic pocket between helices and interferes with the opening and closing of the channel. |
We have now crystallised a bacterial pLIGIC in complex with two commonly used general anaesthetics, desflurane and propofol. The crystal structures were solved using diffraction data collected on beamline ID14-2. They reveal a common binding cavity for the drugs in the membrane bound domain of the “cation channel open” conformation of the protein with interactions between residues that form the cation channel and phospholipids bound to the protein. The cation channel is formed at the interface of the pentamers and the anaesthetics bind in a hydrophobic cleft between four transmembrane helices of each monomer (Figure 101). In order to confirm that this is a physiological relevant binding site, we conducted electrophysiological tests to show that the anaesthetics alter the ion permeability of the channel and that mutations to the residues that form the pocket identified in the crystal structure also alter the response to the drugs. As the pore is opened and closed by relative movements of the helices to which the anaesthetics are bound, their interaction at this site will affect the channels ability to open and close in response to neurotransmitters. The identification of a binding cavity for two of the most commonly used general anaesthetics opens the possibility to develop a new generation of this important class of analgesics with enhanced characteristics.
Principal publication and authors
H. Nury (a,b,c,d), C. Van Renterghem (a,b), Y. Weng (e), A. Tran (e), M. Baaden (f), V. Dufresne (a,b), J. Changeux (b,g), J.M. Sonner (e), M. Delarue (c,d) and P. Corringer (a,b), Nature 469, 428-431 (2011).
(a) Group Recepteurs-Canaux, Institut Pasteur, Paris (France)
(b) CNRS URA 2182, Paris (France)
(c) Unité de Dynamique Structurale des Macromolecules, Institut Pasteur, Paris (France)
(d) CNRS URA 2185, Paris (France)
(e) University of California, San Francisco (USA)
(f) CNRS UBPC UPR 9080, Paris (France)
(g) College de France, Paris (France)
References
[1] N. Bocquet et al., Nature 457, 111-114 (2009).
[2] R.J.C. Hilf et al., Nature 457, 115-118 (2009)



