- Home
- Users & Science
- Scientific Documentation
- ESRF Highlights
- ESRF Highlights 2010
- X-ray imaging
- Tolerance of arteries to microplanar X-ray beams
Tolerance of arteries to microplanar X-ray beams
Radiation-induced damage to healthy tissues limits the maximum dose in the treatment of tumours. It has to be avoided especially for arteries, capillaries and veins because an impaired blood circulation might cause organ dysfunction. The artery wall is a complex structure of multiple layers of elastic fibres, vascular smooth muscle cells (VSMC) and collagen fibres that regulate blood pressure and blood perfusion in organs.
A new radiotherapy protocol micro-beam radiation therapy (MRT) has been developed to spare healthy tissues. X-rays are confined to very thin slices of planar beams of 50 µm arranged in parallel arrays with a interspacing of about 400 µm [1]. As a result, the X-rays irradiate only 20% of a tissue volume, and the areas between the beam slices (valleys) receive less radiation. The microplanar beam arrays are normally cross-fired at the tumour to increase the dose in the valley regions. This therapy has shown in living mice that the cerebral vasculature and the blood brain barrier tolerated high single peak doses (< 1000 Gy) without hemorrhage and loss of blood perfusion [2]. Only at a high peak dose of 1000 Gy, a transient blood brain barrier leakage of 12 days was observed without severe consequences to normal brain function.
We have evaluated the effect of MRT on the artery wall of living mice using intravital microscopic techniques: two-photon microscopy (2PM) and second harmonic generation imaging (SHGI) [3]. A new two-photon imaging protocol was used for a more sensitive and deeper detection of elastic fibres in the artery wall using sulforhodamin-B [4]. In parallel, VSMC in the artery wall were detected after nuclei staining with Hoechst 33342.
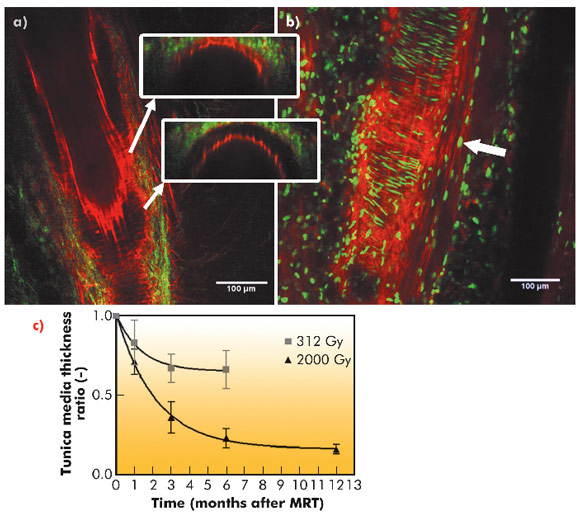
The left hind leg of healthy mice including the saphenous artery was irradiated by an array of 26 microbeams of synchrotron X-rays (50 µm-wide, spaced 400 µm on centre) with peak entrance doses of 312 Gy and 2000 Gy. During 12 months after irradiation, the artery remained patent, but narrow VSMC segments in the tunica media that were in the microplanar beams paths became atrophic and fibrotic in a dose-dependent pattern (Figure 129). The wide tunica media segments between the microbeam paths hypertrophied.
Mice hind leg arteries tolerate microbeam peak doses of up to 2000 Gy delivered by spatially fractioned micro planar beams in a single session without developing occlusions within 1 year, in contrast to the deleterious consequences of comparable doses delivered by broad-beam X-rays. The permanent sequelae of microplanar irradiation appear to be confined to microscopic segments of the tunica media (layer with VSMC) and tunica adventia (outermost collagen layer of the artery that showed fibrosis). Clinical risks of long-delayed disruption or occlusion of non-targeted arteries from microbeam radiation therapy will prove less than corresponding risks from broad-beam radiosurgery, especially if peak doses are kept below 3 hectogray.
Principal publication and authors
B. van der Sanden (a), E. Bräuer-Krisch (b), E. Albert Siegbahn (c), C. Ricard (a), J.-C. Vial (d) and J. Laissue (e), Int. J. Radiation Oncology Biol. Phys. 77, 1545-1552 (2010).
(a) INSERM U836, Institute of Neuroscience, Grenoble (France)
(b) ESRF
(c) Department of Oncology and Pathology, Karolinska Institutet, Stockholm (Sweden)
(d) CNRS UMR 5588, Physical Spectroscopy, Grenoble (France)
(e) Institute of Pathology, University of Bern (Switzerland)
References
[1] D.N. Slatkin, P. Spanne, F.A. Dilmanian and M. Sandborg, Med Phys 19, 1395-1400 (1992).
[2] R. Serduc, P. Verant, J.C. Vial, R. Farion, L. Rocas, C. Remy, T. Fadlallah, E. Brauer, A. Bravin, J. Laissue, H. Blattmann and B. van der Sanden, Int J Radiat Oncol Biol Phys 64, 1519-1527 (2006).
[3] W. Denk, J.H. Strickler and W.W. Webb, Science 248, 73-76 (1990).
[4] C. Ricard, J.C. Vial, J. Douady and B. van der Sanden, J Biomed Opt 12, 064017 (2007).