- Home
- Users & Science
- Scientific Documentation
- ESRF Highlights
- ESRF Highlights 2005
- X-ray Imaging and Optics
- X-ray Microtomography of a Coronary Stent
X-ray Microtomography of a Coronary Stent
Coronary stents are small, metallic scaffolds implanted to re-open coronary arteries which have become seriously narrowed or blocked as a result of heart disease. Re-opening the artery restores blood flow to the heart muscle, reducing the risk of a “heart attack”. A stent is implanted by making a small incision, usually in the femoral artery, through which a guidewire and catheter are inserted, enabling the use of small surgical tools at the blockage site. The stent is crimped onto a special balloon catheter. Once in position, the balloon is inflated with saline, expanding the stent and opening up the blocked artery. The balloon is then deflated and the catheter removed, leaving the stent permanently in place as a support for the artery. Wherever possible, stent implantation is used instead of bypass surgery, because it is much less invasive and the patient can often go home from hospital the same day.
Sometimes, stent implantation is compromised by re-blockage of the artery. This is due to an over-active inflammatory response, triggered by injury to the artery wall during surgery. To prevent re-blockage, the latest stents have a drug coating which suppresses inflammation. Despite the introduction of these drug-coated stents, there is still scope for improving stent design and implantation techniques to reduce vessel injury.
While it is known that stent deployment can injure the vessel wall, it is hard to observe how a stent interacts with the artery during implantation. Detailed observation inside a patient is not yet possible. Imaging in engineering laboratory tests is difficult, because of the small stent size (expanded diameter 3.0 mm; strut width 70-100 µm). The challenge is to find a technique that can image stent deployment, in three dimensions, with a resolution of 10 µm or better so that the interaction of individual struts with the artery can be observed.
Fortunately, a candidate technique exists: X-ray microtomography. This is a development of the computed tomography (CT) technique used in hospitals. The operating principles are the same, except that the resolution attainable is higher. Using the coherent synchrotron X-ray source at the ESRF, volume element (voxel) sizes as small as 0.3 µm are possible and phase contrast techniques can be used to enhance imaging.
An experiment was designed to prove the concept of using X-ray microtomography to study a coronary stent. The stents selected for this study were stainless steel coronary R-stents (Orbus Medical Technologies, Inc.). The experimental setup was kept as simple as possible. Each stent was deployed inside a model artery made from latex rubber and silicone foam, which have similar mechanical properties to natural arterial tissue. Figure 149 shows a stent implanted in a model artery and an X-ray projection taken at the ESRF. Tomography scans were taken before, during and after stent deployment, using beamline BM05. Using 25 keV X-rays, the voxel size was 5.3 µm, with a vertical field of view of 4.5 mm. To image whole stents, which were 13 – 25 mm long, multiple scans were taken, translating the sample vertically between scans until the whole stent was imaged.
 |
|
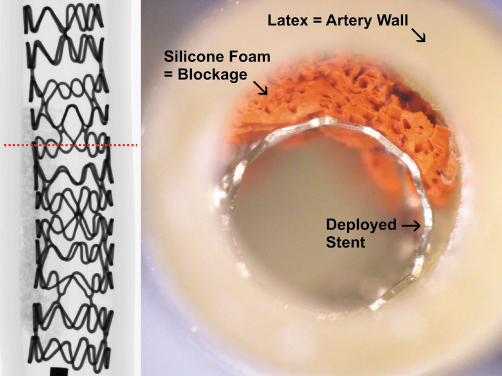
Fig. 149: Photograph of a stent implanted in a model artery. The inset on the left is an X-ray projection of the implanted stent, which is 13 mm long. The dashed line shows the position of the tomography slice shown in Figure 150. |
The tomography data can be observed in a number of ways, such as cross-sections (slices) through the sample, or rendered images. It is also possible to export the data to computer aided design and mechanical modelling software. Figure 150 is an example slice, showing the latex tubing representing the artery wall, the stent struts and the silicone foam representing the blockage. Phase contrast makes it possible to see the foam and the deflated balloon, which was left in place for the scan. The streaks in the image are attenuation artefacts associated with the stent struts. There is a complete set of slices, taken every 5.3 µm, enabling very detailed observation and measurements of stent-artery interactions. Further analysis is in progress.
 |
|
Fig. 150: Example slice from the tomography scan of the stent in Figure 149. |
To conclude, the feasibility of using high-resolution X-ray microtomography to image a coronary stent in a model artery was demonstrated. The stent and artificial artery materials were imaged satisfactorily, though with some attenuation artifacts arising from the metallic stent struts. There is considerable scope to develop the technique further, including observation of real tissue samples or excised stents.
Principal Publication and Authors
T. Connolley (a), D. Nash (a), J-Y. Buffière (b), F. Sharif (a), P.E. McHugh (a), Submitted to Ann. Biomed. Engng.
(a) NCBES, National University of Ireland, Galway (Ireland)
(b) GEMPPM, INSA de Lyon, Villeurbanne (France)



